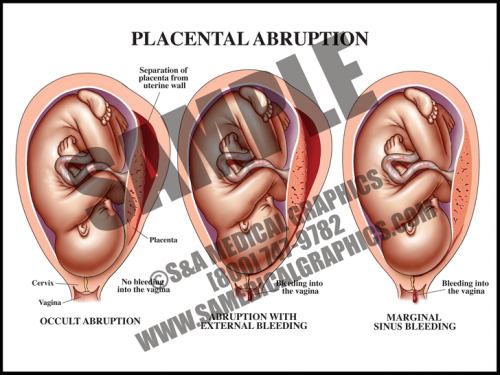
- Abruption occurs when the placenta separates from the uterine wall. Most of the time, this is accompanied by vaginal bleeding as the blood travels between the membranes and the uterus. Some- times, however, there is no bleeding because edges of the placenta remain sealed.
- Symptoms frequently include hypertonic uterus with severe abdominal pain and rapid contractions. If the abruption is large (more than about 50%), the fetus may not survive.
- The specific cause of placental abruption is often unknown, but risk factors include abdominal trauma and maternal factors like smoking, drinking, and diabetes, among others.
- Fetal distress occurs early in this condition in about half of all cases.
-
-
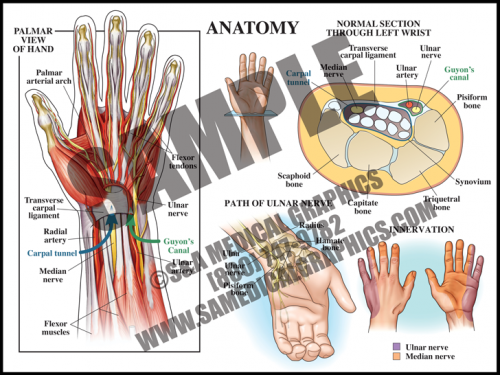
- The carpal tunnel is a passageway on the palmar side of the wrist that houses the median nerve and finger flexor tendons. Anteriorly, the carpal tunnel is bordered by the transverse carpal ligament, a heavy band of fibers that forms the fibrous sheath containing the carpal tunnel; posteriorly, the carpal tunnel is bordered by carpal bones.
- Guyon’s canal contains the ulnar nerve and artery; this anatomy does not pass through the tunnel, but lies superficial to it.
- Carpal tunnel syndrome occurs when the median nerve, which controls sensations to the palm side of the thumb, first, second, and half of the third finger, becomes compressed at the wrist, within the carpal tunnel. This results in pain, weakness, or numbness in the hand and wrist, radiating up to the arm.
-
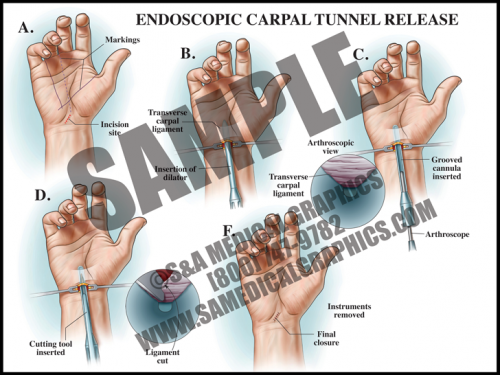
- If conservative treatment is not effective, surgical intervention may be chosen. Surgery can be done as an open procedure or endoscopically.
- In endoscopic surgery, a small incision is made in the wrist and a dilator tube is inserted. An arthroscope with a camera is inserted in order to view the anatomy, then a cutting tool is used to sever the transverse carpal ligament in order to reduce pressure on the median nerve.
- This type of surgery is less invasive and allows for faster recovery and less postoperative pain.
-
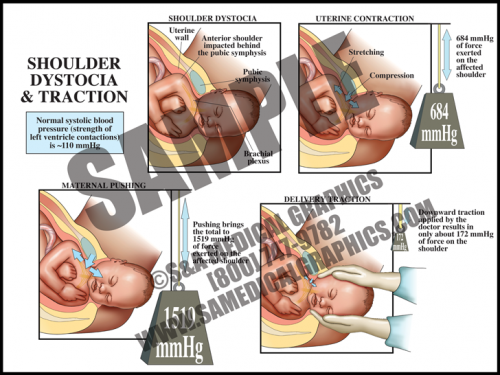
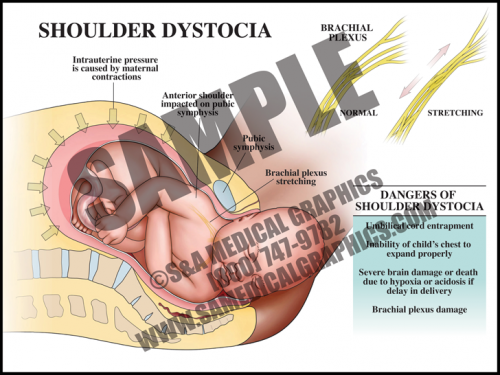
- The uterus itself generates tremendous pressure during contractions. If the average systolic blood pressure (pressure generated by the left ventricle during a contraction) is 120 mmHg, the uterus alone generates more than 5 times that amount. When the accessory muscles (the diaphragm and abdominal muscles) are used to push in conjunction with contractions, this pressure increases to more than 10 times that amount.
- The pull generated by a physician during downward traction for shoulder dystocia is slightly higher than the average systolic blood pressure and contributes only a very small amount to the total amount of generated pressures.
- Uterine and abdominal pressures are good evidence that if shoulder dystocia is the cause of brachial plexus palsy, it is most likely from the intrinsic pressures of the uterus and body wall, not the caregiver.
-
- In 2003, the American College of Obstetrics and Gynecology and the American Academy of Pediatrics recommended adoption of a definition of term intrapartum asphyxia developed by an international task force.
- The definition requires that all four parameters must be met in order to diagnose intrapartum asphyxiation in a term fetus. These include metabolic acidosis, diagnosis of specific types of cerebral palsy correlated with the types of asphyxia damage seen in term fetal brains, early seizures and other neurological signs, and exclusion of all other causes.
- There are other criteria that suggest an intrapartum timing of injury, nonspecific to asphyxia event. These include a hypoxic event immediately before or during birth, sudden, sustained bradycardia or loss of variability along with persistent, late, or variable decelerations, low APGAR scores (<3) beyond 5 minutes, multisystem organ involvement within 72 hours of birth, and early brain imaging showing acute, non-focal cerebral abnormalities.
-
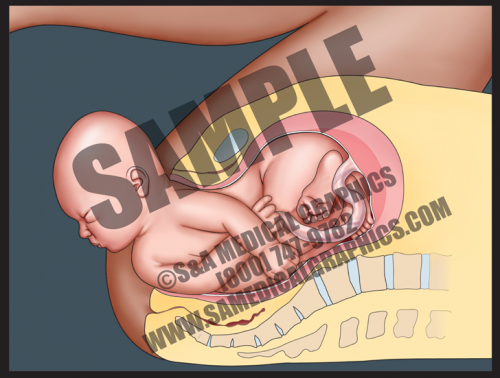
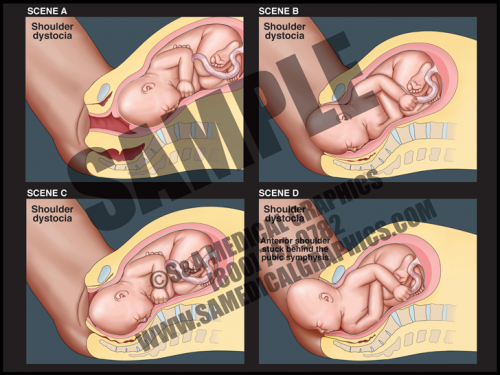
- In cases of shoulder dystocia, the upper fetal shoulder is impacted on the pubic symphysis, or more rarely, the lower shoulder becomes impacted on the sacral promontory or nonexible coccyx. In either case, this event prevents delivery of the baby. Shoulder dystocia can be a potentially catastrophic event since the fetal thorax is still within the pelvis and cannot properly expand for breathing.
- While the rate of shoulder dystocia is higher with gestational diabetic women and macrosomic fetuses (>4500 grams at birth), most cases of shoulder dystocia occur with average-sized fetuses.
- If a brachial plexus palsy (brachioplexopathy) occurs, it usually affects the portions of the brachial plexus that control the shoulder and elbow. Spontaneous recovery is the rule rather than the exception.
- Most fetuses are successfully delivered with a combination of McRoberts maneuver and suprapubic pressure.
-
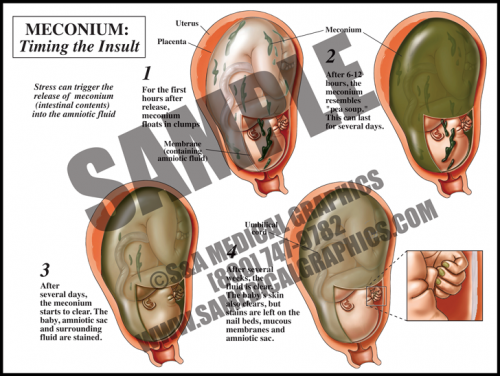
- Meconium is the dark, tarry contents of the fetal gastrointestinal tract. Meconium passage at labor and delivery is common and not a sign of fetal distress unless it is accompanied by other ominous signs.
- Meconium release into the amniotic fluid is however considered a sign of intrauterine fetal distress. This can be caused by placental insufficiency, maternal hypertension, and preeclampsia, among other things.
- When meconium is freshly released, it is clumpy and oats in the amniotic fluid. Within hours, it distributes particulate matter throughout the sac. Macrophages in the fetal skin, mucus membranes, and the amniotic sac phagocytize the particles, giving a green cast to the tissues.
- After several days, the fluid is greenish-brown but clear, and the fetus and membranes are stained. After several weeks, the fetal skin and fluid will clear, but the amniotic membranes, fetal mucus membranes, and nail beds remain stained.
-
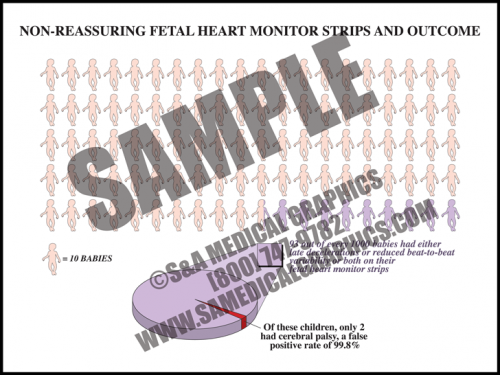
- One risk of fetal heart monitoring technology is false-positive results.
- In fact, “nonreassuring” FHM strips, or those which show either late decelerations, or reduced beat-to-beat variability, or both, have a greater than 99% false-positive rate in predicting cerebral palsy.
-
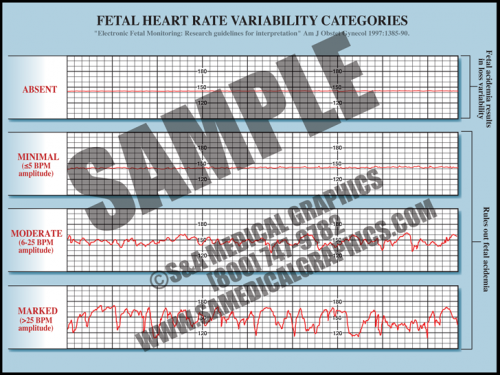
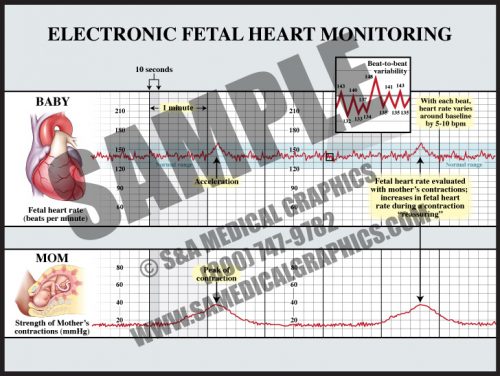
- Fetal heart rate is constantly varying from the baseline; this variability reflects a healthy fetal nervous system and cardiac responsiveness.
- These fluctuations are characterized as absent if there is no variation in the amplitude range, minimal if fluctuation is less than 5 bpm, moderate if fluctuation is 6 to 25 bpm, and marked if fluctuation is greater than 25 bpm.
- Absent variability indicates fetal academia but marked, moderate, and even minimal variation rules it out.
- Conditions like fetal hypoxia, congenital heart anomalies, and fetal tachycardia can cause a decrease in variability.
-
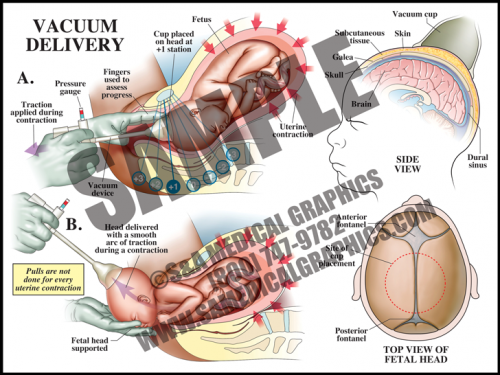
- Vacuum delivery may be performed in cases where there is a prolonged second stage of labor or suspicion of immediate or potential fetal compromise. This procedure assists delivery by helping to move the baby through the birth canal.
- The vacuum cap is a simple device that is placed on the vertex of the head with a small hand-held vacuum pump; some physicians leave the vacuum on between contractions and some release the vacuum. The caps are set to pop off if the vacuum pressure is too high.
- This procedure works with the uterine contractions, gently assisting and guiding the fetus out during contractions, and resting between them. It is not used between contractions.
-
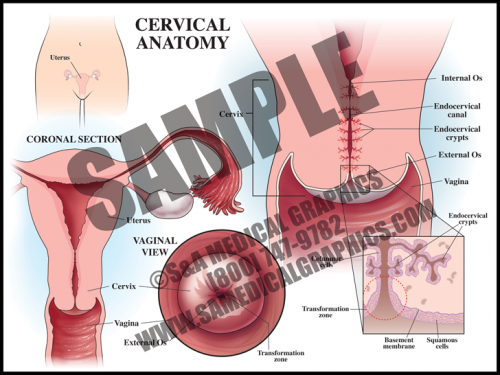
- The cervix is the circular muscle at the base of the uterus; it makes up the top of the vagina.
- The cervical canal passes through the cervix and allows blood from menstruation and a fetus to pass from the uterus into the vagina.
- During a pap smear, a screening test for cervical cancer, cells are scraped from the opening of the cervix and examined under a microscope for abnormality.
- The transformation zone is the area where the mucus secreting columnar cells of the endocervix meet the squamous cells of the ectocervix. Most squamous cell carcinomas and dysplasias are found here.
-
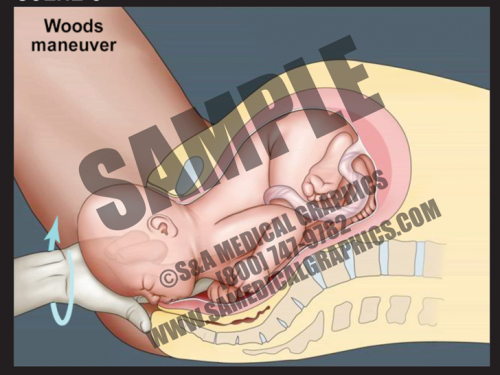
- This 2D dissolve animation shows how this maneuver can release shoulder dystocia impaction and allow for delivery of the fetal shoulder.
- Each animation has pause and play buttons to allow for more interactivity during viewing.
-
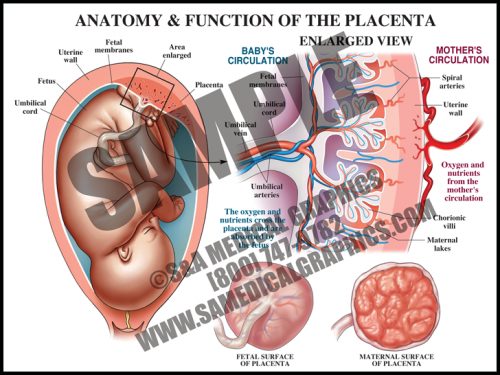
- The placental is a flattened, circular organ that develops in the uterus during pregnancy in order to support the fetus. The fetus is attached to the placenta via the umbilical cord.
- The placenta transfers oxygen and nutrients from the maternal blood to the fetal blood; it also transfers wastes products from the fetal blood to the maternal blood for removal.
- The umbilical cord is normally comprised of three blood vessels, two smaller umbilical arteries that carry deoxygenated blood from the fetus to the placenta, and a larger umbilical vein that supplies the fetus with oxygenated blood from the mother.
- The placenta is expelled from the uterus after the fetus is delivered. Placental pathology can reveal important information about intrauterine conditions and events, as well as shed light on the cause of adverse fetal outcome.
-
- This 2D dissolve animation shows how this maneuver can release shoulder dystocia impaction and allow for delivery of the fetal shoulder.
- Each animation has pause and play buttons to allow for more interactivity during viewing.
-
- This 2D dissolve animation shows how this maneuver can release shoulder dystocia impaction and allow for delivery of the fetal shoulder.
- Each animation has pause and play buttons to allow for more interactivity during viewing.
-
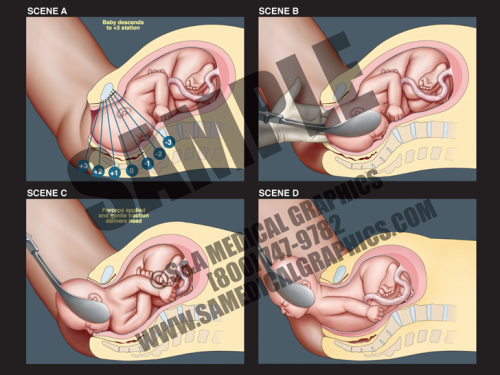
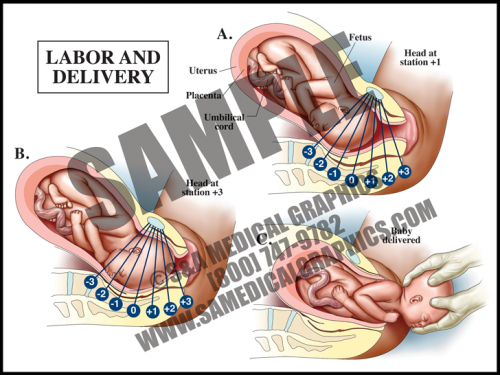
- This 2D animation demonstrates the nor- mal course of labor, showing the dilation of the cervix, descent of the fetus, delivery of the fetal head, and finally delivery of the fetal shoulders and body.
- This animation has pause and play buttons to allow for more interactivity during viewing.
-
- Forceps delivery is a type of operative vaginal delivery performed to help guide the baby out of the birth canal if the second stage of labor isn’t progressing or if fetal safety depends on immediate delivery.
- This 2D animation shows how this procedure is performed, showing that once the fetus has descended far enough down the birth canal, a health care provider applies the forceps to the fetal head.
- The forceps are then used to gently assist and guide the fetus out of the birth canal during uterine contractions. Forceps are not used between contractions.
-
- This 2D dissolve animation shows how this maneuver can release shoulder dystocia impaction and allow for delivery of the fetal shoulder.
- Each animation has pause and play buttons to allow for more interactivity during viewing.
-
- This 2D animation demonstrates how shoulder dystocia occurs during delivery.
- It shows fetal descent down the birth canal and delivery of the fetal head, but impaction of the anterior shoulder on the pubic symphysis, preventing delivery of the shoulder.
- This animation has pause and play buttons to allow for more interactivity during viewing.
-
- In the first stage of labor, the cervix must thin (efface) and open (dilate) to a diameter of about 10 cm (4 in) in order to allow the fetal head to pass through.
- Repeated uterine contractions pushing the fetal presenting part against the inside of the uterus cause the cervix to thin and open over time.
- The fetal presenting part is considered to be engaged when the lowest portion is at the level of the ischial spines; this is called the 0 station. Fetal movement down the birth canal is measured by positive stations, using a 0/+3 scale or a 0/+5 scale.
- The second stage of labor starts at full dilation of the cervix and is completed when the fetus is delivered. The third stage is the delivery of the placenta.
-
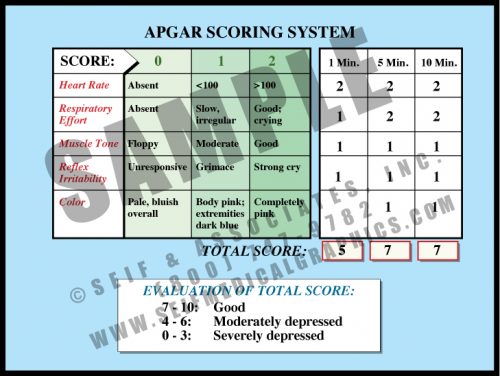
- This simple scoring system indicates how well the fetus fared through labor and delivery. The maximum score is 10 and the minimum is 0, with up to 2 points being awarded for each of 5 measures of health.
- Apgar scoring is done at 1 minute and 5 minutes of age, sometimes by nursing staff, sometimes by physicians. If the 5-minute score is low, a 10, 15 or 20-minute score may be recorded, either until the baby is stable or moved from the delivery room for specialized care.
- While there is some correlation between low 5 minute Apgar scores and neurological outcome, only a very small percentage of children with low 5 minute scores sustain brain damage. The longer the score remains low, the higher the correlation with neurological damage.
-
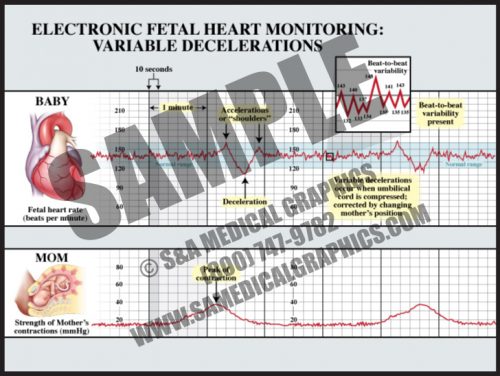
- Variable decelerations can occur at any time during or between contractions and are usually characterized by “shoulders” before and sometimes after the deceleration.
- The decelerations are usually “V” or “U”-shaped and return to baseline within two minutes or less.
- Variable decelerations are due to head or cord compression and are “treated” by changing the mother’s position and applying oxygen.
- Unless very deep (<60 bpm) for extended periods (>2 minutes or more), they are considered benign.
- Variable decelerations occur during the second stage of most labors, as the fetal head moves down the narrow vaginal canal and is compressed by a combination of the uterine contractions and the narrow vagina.
-
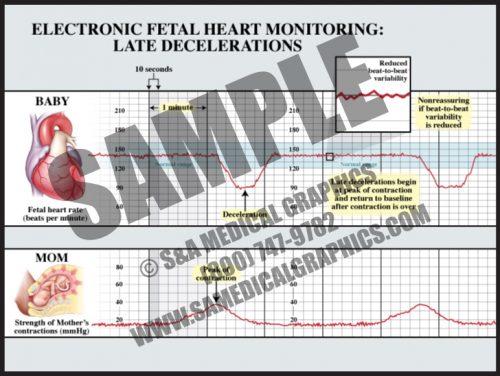
- Late decelerations start at or after the peak of a contraction and are considered to be a sign of uteroplacental insufficiency.
- The depth of late decelerations is probably not as significant as their presence. If frequent, they can be a sign of fetal distress and an indication for prompt delivery.
- If late decelerations are accompanied by loss of beat-to-beat variability, it is generally considered an indication for urgent or emergent delivery, either by cesarean section or operative delivery (forceps or vacuum extraction), depending upon the state of the labor.
- The vast majority of fetuses with nonreassuring fetal heart tracings are completely normal.
-
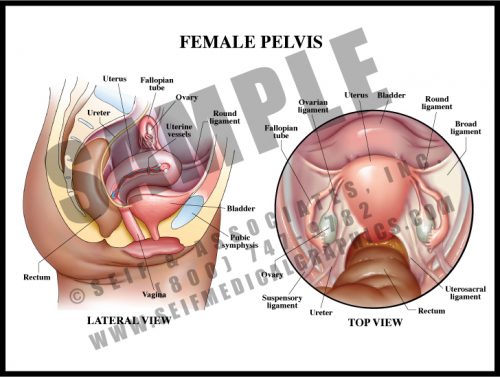
- The female pelvis contains the bladder, uterus, vagina, and rectum. The tissue between the vaginal and rectal openings is a tight collection of tendons from the pelvic floor muscles, the perineum. The entire region is called the vulva.
- The non-pregnant uterus is about the size of a small pear. It is a hollow muscular organ, its neck enclosed by a thick circular muscle known as the cervix.
- Urine is excreted from the kidneys via the ureters, which transport it to the bladder. It is then carried to the outside by the relatively short urethra.
- The ovaries release ova (eggs) each month to the uterus via the fallopian tubes; ovarian hormones are absorbed into the bloodstream.
- The organs are held in the pelvis by a number of ligaments connecting them to the pelvic walls.
-
- This technology, used in approximately 87% of all labors in the U.S., tracks the fetal heart function against uterine contractions.
- The normal fetal heart rate is approximately 120-160 beats per minute (bpm), although normal individual fetuses might be higher or lower than this range.
- Beat-to-beat variability is literally the changes of the fetal heart rate from beat to beat (short-term variability), and within 3-5 minute periods (long-term variability). Beat-to-beat variability decreases or disappears for 20-30 minute time periods as the fetus sleeps, but is present in most normal labors and represents the health of the fetal brainstem.
-
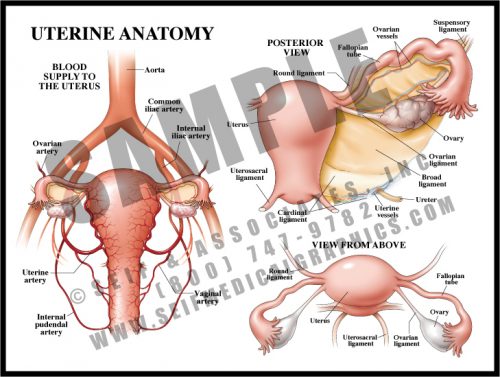
- The uterus is small and contracted in its non-pregnant state, but grows to fill nearly the entire abdomen during pregnancy. Delivery is effected by repeated strong contractions pushing the fetus through the cervix and out the birth canal (vagina).
- The fallopian tubes carry the ova to the uterine cavity, where fertilized eggs implant and develop.
- The blood supply to the uterus is redundant and increases greatly during pregnancy.
-
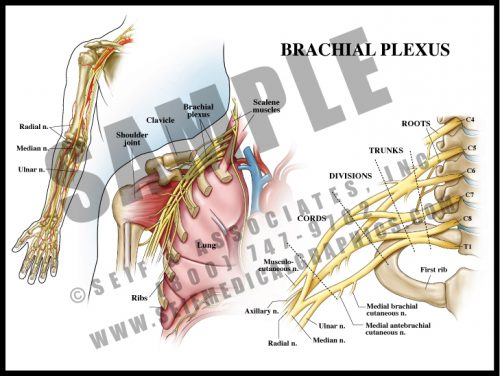
- The nerve roots of the lower cervical spinal cord split and merge several times before supplying the arm and hand.
- The brachial plexus lies over the first rib and behind the clavicle. It is intimately related to the subclavian/brachial artery and passes between the scalene muscles of the neck.
- The plexus is divided into roots, trunks, divisions, cords and terminal branches. By looking at the anatomical distribution of pain or dysfunction, it is possible to determine the location of a brachial plexus lesion.
- Brachial plexopathy can occur during delivery with or without shoulder dystocia, and from thoracic outlet syndrome.
-
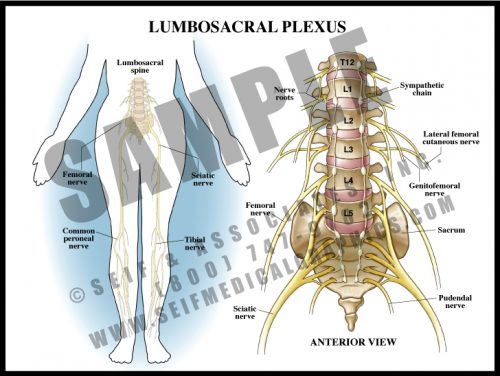
- Analogous to the brachial plexus, the lumbosacral plexus is a series of nerve convergences and separations which ultimately combine into several large terminal nerves.
- Plexi form a protective mechanism in that if one nerve root is damaged, a particular muscle might be weakened, but function would not be completely lost.
- The terminal nerves in the legs generally follow the course of the deep vasculature.
- Terminal sensory nerves to the feet are particularly vulnerable to diabetes, resulting in peripheral diabetic neuropathy. This frequently contributes to foot infections and the need for amputation.
-
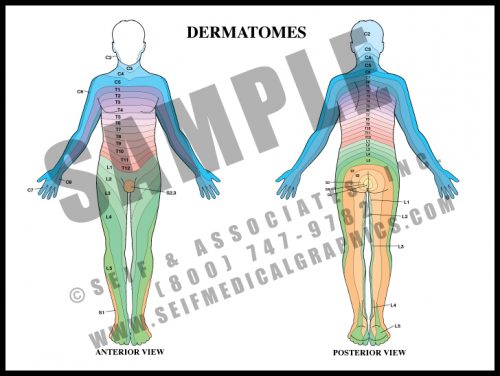
- Dermatomes are strips of skin which are supplied by the nerve roots. If there is numbness or pain along a dermatome, it is a sign of damage or irritation of a specific nerve root, where the root exits the spinal cord and vertebral column. This is known as radiculopathy.
- Soon after the cervical and lumbosacral nerves leave the cord, they join and separate several times (plexi) before reaching their target organs. Nerve fibers to a given muscle may come from several different nerve roots. The skin sensory supply, however, remains directly associated with the root alone.
- Radicular pain usually occurs with compression of the nerve in the foramen, the hole by which the nerve exits the spinal canal.
-
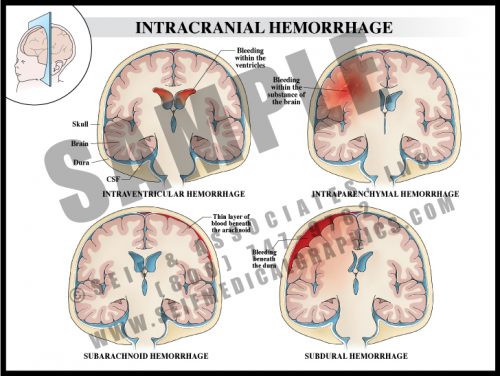
- Intraventricular hemorrhage is bleeding within the cavities of the brain that normally hold clear cerebrospinal fluid (CSF). Such bleeding is frequently associated with pre-term delivery and can result in hydrocephalus and loss of brain tissue.
- Intraparenchymal bleeding is within the brain tissue itself and usually results from ruptured arteriovenous malformation (AVM), hemorrhage following ischemic infarction or hypertension.
- Subarachnoid hemorrhage usually results from a ruptured surface AVM or cerebral artery aneurysm.
- Subdural hemorrhage is the result of trauma leading to disruption of bridging veins between the dura and the brain.